Expert diagnosis and treatment in Hampshire
As a consultant cardiologist with triple accreditation in cardiac imaging, Dr Cassar sees many patients who’ve been diagnosed with atrial fibrillation but remain confused about what it actually means for them. AF is indeed common – affecting over a million people in the UK – but each person’s situation is different. Dr Cassar’s approach focuses on comprehensive cardiac imaging to understand not just that you have AF, but why you have it and what that means for your treatment.
Atrial fibrillation (AF) is a heart rhythm disorder characterised by rapid, irregular electrical activity in the heart’s upper chambers (atria). Instead of the coordinated contraction that occurs with normal heart rhythm, the atria quiver chaotically at rates of 300-600 beats per minute. This disorganised activity prevents effective atrial contraction and causes an irregularly irregular pulse, often with a fast ventricular rate. AF may occur in episodes (paroxysmal AF), persist for more than seven days (persistent AF), or become permanent.
Multiple factors can trigger or predispose to atrial fibrillation. Age represents the strongest risk factor, with AF prevalence increasing significantly after 65 years. High blood pressure, coronary artery disease, heart valve problems, heart failure, and thyroid disorders all increase AF risk. Excessive alcohol consumption, particularly binge drinking, can precipitate episodes. Other contributing factors include sleep apnoea, obesity, diabetes, and lung disease. Some individuals develop AF without identifiable underlying heart disease, termed lone atrial fibrillation, though this becomes less common as patients age and other conditions emerge.
Atrial fibrillation carries important health implications beyond the rhythm disturbance itself. The most serious concern is stroke risk: AF increases stroke risk five-fold because blood can pool and clot in the quivering atria, with clots potentially travelling to the brain. AF also commonly causes troublesome symptoms including palpitations, breathlessness, fatigue, and reduced exercise capacity that significantly impact daily activities. Over time, poorly controlled AF can weaken the heart muscle, leading to heart failure. The irregular heart rhythm may also cause anxiety and sleep disturbance, affecting overall wellbeing and quality of life.
Awareness of fast, irregular, or 'fluttering' heartbeat that may come and go or persist continuously
Shortness of breath with exertion or at rest, particularly during AF episodes or with fast heart rates
Reduced energy levels, feeling tired easily, and decreased ability to perform usual physical activities
Difficulty with exercise or activities that were previously manageable, particularly if heart rate rises rapidly.
Feeling faint, dizzy, or lightheaded, especially when AF occurs with very fast or slow heart rates.
Chest tightness, discomfort, or pressure during episodes, though severe chest pain is uncommon with AF alone
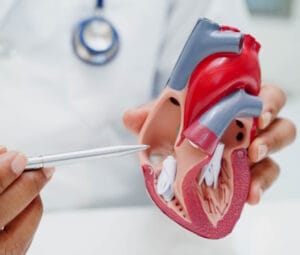
Diagnosing AF starts with understanding your symptoms and their pattern. Are your palpitations constant or do they come and go? Do they last seconds, minutes, or hours? Are there triggers like alcohol, caffeine, or stress? These details help determine whether you have paroxysmal AF (episodes that come and go), persistent AF (continuous episodes lasting over a week), or permanent AF. During examination, feeling your pulse reveals the characteristic irregularly irregular rhythm of AF – the heartbeat has no pattern, distinguishing it from other rhythm problems. Blood pressure measurement and cardiovascular examination check for signs of heart strain, valve problems, or fluid retention that might complicate AF or indicate underlying causes.
An electrocardiogram (ECG) confirms AF by capturing the characteristic disorganised and irregular rhythm of AF. However, if your symptoms come and go, a standard ECG might miss episodes entirely. This is where ambulatory monitoring becomes valuable: a 24-hour Holter monitor records every heartbeat for a day, whilst longer-term event recorders (worn for weeks) capture infrequent episodes. Some patients experience palpitations weekly or monthly, making these extended monitors essential for diagnosis.
Blood tests check for reversible causes: an overactive thyroid can trigger AF, whilst kidney problems or electrolyte imbalances might complicate treatment. Dr Cassar’s imaging expertise becomes particularly important during echocardiography – detailed ultrasound assessment identifies whether AF has caused heart muscle weakening, whether valve disease might be triggering AF, or whether the heart’s upper chambers have enlarged (suggesting longstanding AF). These findings directly influence treatment decisions.
Once AF is confirmed, stroke risk assessment becomes crucial. This is done by using a validated risk score that combines age, medical conditions, and previous strokes – determining whether blood-thinning medication is recommended. Higher scores mean higher stroke risk and clearer benefit from anticoagulation.
However, blood thinners increase bleeding risk, so Dr Cassar also considers factors like previous bleeding episodes, falls risk, and kidney function. This balancing act between preventing stroke and avoiding bleeding complications requires individualised assessment rather than rigid protocols. For some patients, additional imaging with transoesophageal echocardiography (an ultrasound probe passed down the gullet to look directly at the heart) may be needed before cardioversion procedures to ensure no clots have already formed.
Dr Cassar’s approach integrates all these findings – symptom pattern, ECG and monitoring results, blood tests, detailed cardiac imaging, and risk scores – to develop a comprehensive treatment plan addressing stroke prevention, rhythm or rate control, and any underlying cardiac conditions contributing to your AF.
Atrial fibrillation management focuses on three key objectives: preventing stroke through anticoagulation, controlling heart rate or restoring normal rhythm, and addressing underlying conditions. Treatment approaches are personalised based on your AF pattern, symptoms, stroke risk, and individual circumstances. Dr Cassar works with you to develop a comprehensive management plan that optimises your cardiovascular health and quality of life.
Addressing modifiable risk factors significantly improves AF management outcomes. Weight loss benefits overweight individuals, with studies showing AF burden reduction or resolution following substantial weight loss. Alcohol moderation is crucial, as even moderate alcohol consumption increases AF risk and episodes. Blood pressure optimisation, sleep apnoea treatment, and diabetes management all improve AF control. Regular exercise, whilst generally beneficial for cardiovascular health, should be moderate as extreme endurance exercise may increase AF risk. Managing underlying conditions including thyroid disorders, heart valve disease, and coronary artery disease addresses AF triggers. Stress management, adequate sleep, and avoiding excessive caffeine can reduce episode frequency. Comprehensive lifestyle modification, combined with appropriate medical therapy, optimises AF management and potentially reduces the need for more invasive interventions.
Stroke prevention represents the most important aspect of AF management, as anticoagulation therapy dramatically reduces stroke risk. For most patients with AF and risk factors for stroke, anticoagulation is recommended. Direct oral anticoagulants (DOACs) offer effective stroke prevention with lower bleeding risk compared to warfarin and don’t require regular blood test monitoring. Warfarin remains appropriate for some patients, particularly those with mechanical heart valves or severe kidney impairment. Anticoagulation decisions balance stroke risk against bleeding risk, considering factors such as age, falls risk, previous bleeding, and kidney function. Regular review ensures anticoagulation remains appropriate and well-tolerated, providing crucial protection against devastating stroke complications.
The choice between rate control and rhythm control isn’t always obvious from guidelines alone. A 45-year-old with paroxysmal AF and significant symptoms is very different from a 75-year-old with permanent AF who feels fine. The ‘110 beats per minute (bpm)’ target mentioned in guidelines is helpful, but patients’ tolerance varies considerably – some feel unwell at 95 bpm whilst others remain comfortable at 115 bpm during activities. Dr Cassar uses comprehensive assessment, including heart rate monitoring when needed, to tailor treatment to each patient’s specific circumstances and symptom profile. Rate control combined with blood thinning medication (anticoagulation) provides effective management for many AF patients.
Rhythm control strategies aim to restore and maintain normal heart rhythm, potentially eliminating AF symptoms. Electrical cardioversion delivers a controlled electrical shock to reset heart rhythm, whilst pharmacological cardioversion uses anti-arrhythmic medications. Cardioversion is particularly effective for recent-onset AF or persistent AF causing significant symptoms. However, requiring anti-arrhythmic medications to maintain normal rhythm. The ‘pill-in-the-pocket’ approach allows some patients with infrequent paroxysmal AF to take medication only when episodes occur. Rhythm control suits younger, symptomatic patients and those with recent-onset AF, though success rates decline with longstanding AF and significant atrial enlargement. Careful patient selection and realistic expectation-setting optimise outcomes.
Patients frequently ask whether they ‘need’ ablation. The honest answer is that ablation is only one tool in the arsenal of a cardiologist – AF can often be managed with medications. However, for younger, active patients whose quality of life is significantly impacted by AF despite drugs, ablation offers a realistic chance of long-term freedom from episodes. Dr Cassar discusses success rates candidly: around 70-80% for first-time paroxysmal AF ablation, dropping to 50-60% for persistent AF, with some patients requiring a second procedure. It’s not a guaranteed cure, but for appropriately selected patients, it can be transformative. Dr Cassar works closely with specialist electrophysiologists when ablation is the right choice, ensuring patients receive expert procedural care. Left atrial appendage occlusion devices offer an alternative stroke prevention strategy for patients unable to tolerate anticoagulation.
Everyone experiences AF differently. Many people notice their heart fluttering, racing, or feeling like it’s skipping beats. You might feel out of breath, especially when doing everyday activities, or find yourself getting tired more easily than usual. Some people feel dizzy or lightheaded. However, not everyone has symptoms; some discover their AF during a routine check-up. If your heartbeat feels unusual or worrying, it’s worth getting checked out.
AF happens when the electrical signals in your heart become disorganized, causing the upper chambers to beat chaotically instead of in a regular rhythm. Several things can lead to this. High blood pressure is the most common cause; it makes your heart work harder and can stretch the heart chambers over time. Other heart conditions like valve problems, coronary artery disease, or previous heart attacks can trigger AF. Age is a major factor too; the older you get, the more likely you are to develop AF. Other causes include an overactive thyroid gland, sleep apnoea (where breathing stops and starts during sleep), excessive alcohol use, obesity, and diabetes. Sometimes AF develops without any obvious cause, particularly in younger people, though this is less common.
AF can run in families, but it’s not inherited in a straightforward way like eye colour. If you have a parent or sibling with AF, your risk is higher – roughly 40% higher than someone without a family history. However, having AF in your family doesn’t mean you’ll definitely get it. Many people develop AF without any family history, and many people with relatives who have AF never develop it themselves. The genetic link is complex and likely involves multiple genes working together with lifestyle factors. If AF runs in your family, it’s even more important to control risk factors you can change – like keeping your blood pressure down, maintaining a healthy weight, limiting alcohol, and staying active.
AF rarely disappears completely by itself. Some people have episodes that start and stop on their own, but the underlying condition usually remains. Without treatment, AF typically gets worse over time – occasional episodes can become more frequent or constant. Even if you stop feeling symptoms, the risk of stroke remains high unless you’re on proper treatment. The good news is that with the right medication and lifestyle changes, we can control AF and often prevent it from getting worse.
AF does increase stroke risk, but how much depends on your individual circumstances. The often-quoted “five times higher risk” applies to average populations, but your personal risk varies greatly depending on factors like your age, blood pressure, diabetes, and previous strokes. Some people with AF have very low stroke risk (less than 1% per year), whilst others have higher risk. This is why your doctor calculates your personal risk score to determine whether you need blood thinners. AF can also weaken your heart over time if left uncontrolled. The important message is that with appropriate treatment tailored to your individual risk – which may include blood thinners, heart rate medication, and lifestyle changes – we can manage AF effectively and most people live full, active lives.
Most people with AF need blood thinning medication to prevent strokes. Your doctor will assess your personal stroke risk based on your age and other health conditions like high blood pressure or diabetes. Modern blood thinners (called DOACs) are much easier to take than the old warfarin – they work well, have fewer side effects, and don’t require regular blood tests. Your doctor will weigh up your stroke risk against any bleeding risk to decide what’s right for you.
Your doctor will start by asking about your symptoms and checking your pulse for irregular beats. An ECG (a simple heart tracing) confirms the diagnosis – it takes just a few minutes and doesn’t hurt. If your AF comes and goes, you might wear a heart monitor at home for 24 hours or longer to catch episodes. Blood tests check your thyroid and other factors that can affect your heart. An ultrasound scan of your heart (echocardiogram) shows how well your heart is pumping and checks for other problems.
Think of it this way: rate control keeps your heart from beating too fast during AF, but allows the irregular rhythm to continue. You take daily medication (usually beta-blockers) and your heart stays in AF but at a safer, slower rate. This works well for many people. Rhythm control tries to get your heart back into normal rhythm using stronger medications or procedures. It’s like trying to fix the problem rather than just managing it. Your doctor will recommend which approach suits you best based on your symptoms and circumstances.
Catheter ablation is a procedure that can stop AF by blocking the abnormal electrical signals in your heart. Doctors insert thin tubes through blood vessels in your groin and use them to create tiny scars in specific areas of your heart. It works best for people whose AF comes and goes, with success rates around 70-80%. You might consider ablation if medications aren’t working well, if you want to avoid taking drugs long-term, or if AF is weakening your heart. It’s worth noting that even after successful ablation, most people still need blood thinners if their stroke risk is high.
Common triggers include drinking too much alcohol (especially binge drinking), caffeine, stress, poor sleep, and becoming dehydrated. Some people find that large or heavy meals set off episodes. Everyone’s different though. Try keeping a simple diary of when your AF happens and what you were doing beforehand; this can help you spot your personal triggers and avoid them.
Yes, absolutely. If you’re overweight, losing weight is one of the best things you can do for your AF. Studies show that losing just 10% of your body weight can reduce AF episodes by up to 60%. Weight loss also helps with high blood pressure, sleep problems, and diabetes – all of which make AF worse. Combined with moderate exercise and cutting back on alcohol, weight loss can sometimes reduce or even eliminate the need for stronger treatments.
Yes, most people with AF should exercise. Regular moderate activity is good for your heart and overall health. Start slowly and build up gradually – even 10 minutes of walking is a good start. Talk to your doctor before beginning any exercise program, especially if you feel symptoms during activity. While moderate exercise helps, very intense endurance training might actually increase AF risk, so balance is key.
AF usually progresses without treatment. Episodes that start occasionally often become more frequent or last longer. Eventually, AF can become constant. This happens because AF causes changes in your heart that make more AF more likely – it’s a bit of a vicious cycle. But here’s the good news: early treatment, lifestyle changes, and regular monitoring can slow down or even prevent this progression.
While your GP can start basic treatment, a heart specialist (cardiologist) ensures you get the most up-to-date, comprehensive care. A specialist can accurately assess your stroke risk, arrange detailed heart scans, discuss all treatment options including procedures, and make sure you’re on the best treatment plan for your individual situation. Complex decisions about blood thinners and whether to try restoring normal rhythm benefit from specialist expertise.
Dr Cassar is a consultant cardiologist seeing patients in Basingstoke and Winchester. He has extensive experience managing AF and specialized training in heart imaging, including advanced scans that show exactly what’s happening with your heart. He’ll take time to understand your symptoms and concerns, assess your individual risks, and work with you to create a treatment plan that fits your life. If you need specialized procedures like ablation, he can arrange referrals to the best electrophysiology teams.
Dr Cassar will want to hear about your symptoms – when they happen, what they feel like, and how they affect your daily life. He’ll check your pulse and blood pressure and examine your heart. Depending on what you need, he might arrange an ECG, blood tests, or a heart scan. You’ll discuss your stroke risk and all your treatment options in plain English. The aim is to create a clear plan that gives you confidence about managing your AF and reduces your risk of complications.
You can contact Dr Cassar’s practice directly to arrange an appointment. He sees patients at Candover Clinic in Basingstoke and in Winchester. Getting specialist assessment early means you’ll get the right tests, understand your personal risks, and start the most effective treatment sooner.
There are excellent resources to support you in managing atrial fibrillation: